Rev. OFIL 2017, 27;2:210-212
Fecha de recepción: 14/06/2016 – Fecha de aceptación: 15/10/2016
Carnero Gregorio M1, Torres Crigna A2, Carnero Gregorio O2, Corbalán Rivas A2, Rodríguez Cerdeira C3
1 Departamento de Bioquímica, Genética e Inmunología. Universidad de Vigo (España)
2 Asociación Española de Pacientes con Glicogénesis (España)
3 Departamento de Dermatología. CHUVI y Universidad de Vigo (España)
Correspondencia:
Miguel Carnero Gregorio
Universidad de Vigo
(Departamento de Bioquímica, Genética e Inmunología)
Prexigueiro, 70
32418 Ribadavia – Ourense
Correo electrónico: miguel.carnero.gregorio@hotmail.com
____
SUMMARY
Introduction and objectives: Infections are common in glycogen storage disease type Ib (GSD Ib) patients due to associated chronic severe neutropenia. Immunonutrition might help to minimize infections in these individuals. The aim is to compare the count of respiratory infection episodes in a GSD Ib patient, before and during a supplementary nutritional treatment.
Materials and methods: A retrospective case report study in a 42-year-old male GSD Ib patient. The supplementary nutritional treatment began in June 2002. A period of 20 years was evaluated: 10 years prior to the beginning of the treatment as well as the 10 years of the actual treatment. No other dietary or therapeutic modifications were made.
Results and discussion: Seven respiratory infections were recorded before the treatment. In all cases, antibiotic therapy as well as granulocyte-colony stimulating factor (G-CSF) were needed for the complete remission of infections. No airway infections that involved medical care or treatment were recorded in the post-treatment period.
Conclusion: Immunonutrition could help reduce the number of respiratory complications in GSD Ib patients.
Key Words: Glycogen storage disease, nutritional supplements, impact, inmunonutrition, respiratory infections.
____
INTRODUCTION AND OBJECTIVES
Glycogen storage disease (GSD) is a group of metabolic disorders that include those related to glycogen metabolism. At present, 16 types are known, from 0 to XV, each having different degrees of severity and impact on organs1. In hepatocytes, there is a pathway that transforms glucose-6-phosphate (G6P) into glucose. The malfunction of this pathway leads to GSD I with a very low prevalence (about 1:100,000–1:300,000 cases). In this disorder, subtype Ib affects 20% of patients. Some of the symptoms manifested are hypoglycemia, hypertriglyceridemia, hyperuricemia and neutropenia. Due to this severe chronic neutropenia, recurrent infections are frequent in these patients, including those in the respiratory tract, wich are between the most common ones2.
Currently, there are multiple studies on immunomodulatory diets and their capacity to stimulate the immune system3,4. At this time, no consensual conclusions have been reached on the beneficial effects in different pathologies.
Authors agree that some nutrients may help reduce the number of infections. Arginine (Arg) is one of the nutrients which may be effective in reducing infections of the upper respiratory tract5,6.
The number of myeloid suppressor cells (MDSC) increase in response to certain disorders: cancer, autoimmune diseases, acute and chronic infections and stress. MDSC have a role in reducing the immune response. Moreover, MDSC regulate the availability of arginine needed for the normal function of T lymphocytes7. Nutritional supplements containing arginine and omega-3 fatty acids (ω-3), seem to neutralize the regulatory effects of MDSC8.
Arg is transformed into nitric oxid (NO) that, when in deficit, impairs blood microcirculation9.
Arginine supplementation improves both wound healing and immune function by ameliorating the function of T cells, often associated with traumas. Oral administration of 30 g of this amino acid in human volunteers gives rise to an increase in lymphocyte blastogenic transformation when stimulated by mitogens10.
This report focused on the observation of respiratory tract infections due to it was the only patient’s disease condition which was influenced by the introduction of nutritional supplement discussed here.
The aim was to compare the count of respiratory tract infections in a 42-year-old patient with GSD Ib, both before and during the use of an oral nutritional supplement containing Arg.
MATERIALS AND METHODS
Retrospective case report study of a 42-year-old patient affected by GSD type Ib. Related with his main pathology, the following chronic items are actives in the patient: neutropenia, gastroesophageal reflux disease, like-Cronh inflammatory bowel disease, periodic furunculosis, nephrolithiasis, osteopenia and rarely iron deficiency anemia. Other not GSD related active disease: bilateral sensorineural deafness Medical records of all respiratory tract infection episodes were collected. The number of other infection episodes was lower in comparation with the respiratory tract infections, so we only determine those ones.
Impact® enteral (Nestlé Health Science©, Switzerland) was used as the nutritional supplement treatment, with a 250 mL dose in the morning and at night. The total arginine amount per day was 6.25 g. Impact® enteral also contains other immunonutrients as omega-3 fatty acids (1.7 g/L) and dietary nucleotides (1.2 g/L).
The supplementation started in June 2002. A period of 20 years was evaluated: 10 years prior to the beginning of the supplementation (1993-2002) as well as the 10 years of the actual supplementation (2003-2012). No other dietary or therapeutic modifications were made.
RESULTS AND DISCUSSION
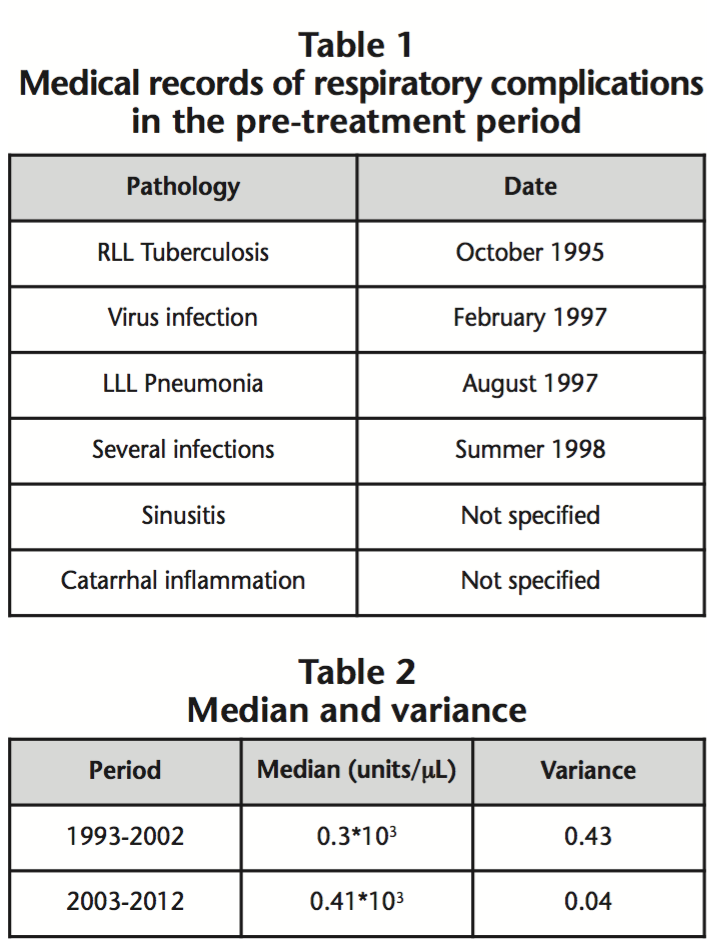
The count of respiratory complications in the patient’s medical records in the 10-year period prior to treatment was five: tuberculosis in RLL (right lower lobe), pneumonia in LLL (Left lower lobe), sinusitis, an undetermined count of respiratory tract and tonsil infections and cold symptoms with fever and yellowish expectoration lasting 5 days. Dates can be seen in table 1.
Oral antibiotics and treatment with granulocyte colony-stimulating factor (G-CSF) were administered for the remission of the infections in all of the above cases.
In the period of supplementation with Impact® enteral no respiratory tract infections requiring medical assistance or treatment were recorded. The patient experienced only two common colds during the 10-year treatment.
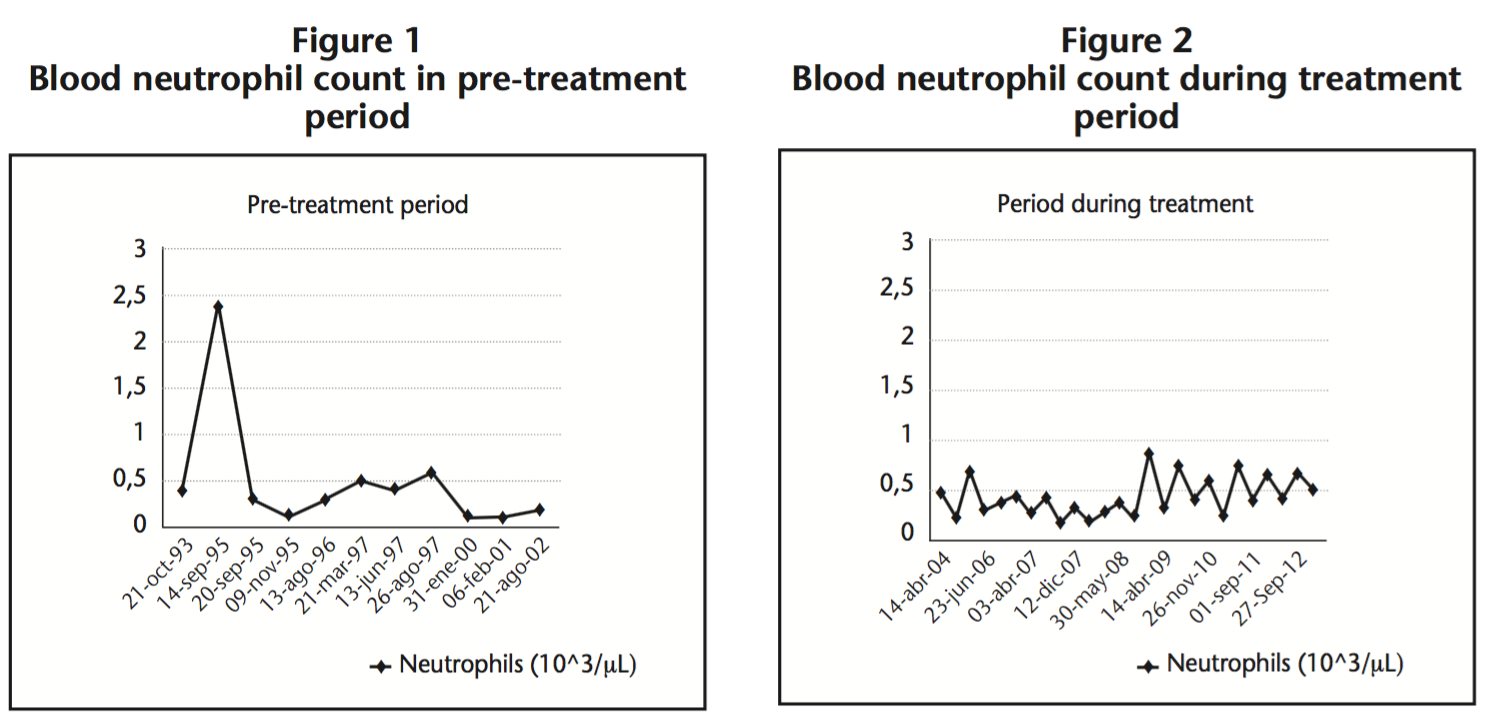
As shown in figures 1 and 2, once on treatment with nutritional supplement, the variation of neutrophil count showed a noticeable increase.
The median and variance of both periods can be seen in table 2.
This study covers the adult stage of the patient’s life between the age of 21 and 40. Throughout the full 20-year period, the patient has been living in the same city, has maintained the same eating habits and has been on the same prolonged pharmacological therapy. Therefore, no other known factors have intervened in the individual.
CONCLUSION
Data show an improvement in the patient’s immune system once on the nutritional supplement. The use of immunonutrition in the diet of GSD Ib patients might help to reduce the count of respiratory infections due to chronic neutropenia. Keeping a close watch on the total count of neutrophils is a good marker in assessing the effectiveness of this type of supplements.
More studies with a cohort of patients is needed to validate arginine as a supplementary immunonutritional therapy.
Conflict of interest: The authors declare no conflicts of interest.
BIBLIOGRAPHY
1. Chen Y (2001) Glycogen storage diseases. In: Scriver C, Beaudet A, Sly W, et al. (eds) The Metabolic and Molecular Bases of Inherited Disease. McGraw-Hill, New York, pp 1521-1555.
2. Visser G, Rake JP, Fernandes J, et al (2000). Neutropenia, neutrophil dysfunction, and inflammatory bowel disease in glycogen storage disease type Ib: results of the European Study on Glycogen Storage Disease type I. J Pediatr. 137:187-191. doi: 10.1067/mpd.2000.105232.
3. Słotwiński R, Słotwińska S, Kędziora S, Bałan BJ (2011). Innate immunity signaling pathways: links between immunonutrition and responses to sepsis. Arch Immunol Ther Exp. (Warsz) 59:139-150. doi: 10.1007/s00005-011-0117-2.
4. Zapatera B, Prados A, Gómez-Martínez S, Marcos A (2015). Immunonutrition: methodology and applications. Nutr Hosp. 31 Suppl 3:145-154. doi: 10.3305/ nh.2015.31.sup3.8762.
5. Barbul A (1990) Arginine and immune function. Nutr Burbank Los Angel Cty Calif. 6:53-58; discussion 59-62.
6. Drover JW, Dhaliwal R, Weitzel L, et al. (2011). Perioperative use of arginine-supplemented diets: a systematic review of the evidence. J Am Coll Surg. 212:385-399, 399.e1. doi: 10.1016/j.jamcollsurg. 2010.10.016.
7. Gimeno R, Barquinero J (2011). Myeloid-derived suppressor cells (MDSC): Another player in the orchestra. Inmunología 30:45-53.
8. Marik PE, Flemmer M (2012). The immune response to surgery and trauma: Implications for treatment. J Trauma Acute Care Surg. 73:801-808. doi: 10.1097/ TA.0b013e318265cf87.
9. Popovic PJ, Zeh HJ, Ochoa JB (2007). Arginine and immunity. J Nutr. 137:1681S-1686S.
10. Culebras-Fernández JM, De Paz-Arias R, Jorquera-Plaza F, others (2001). Nutrición en el paciente quirúrgico: inmunonutrición.
____
Download PDF: Reducing frequency in respiratory infections in glycogen storage disease Ib with a nutritional supplement. Case report
